AUTOMEDIQ

Problem
Challenges in Manual Processing of Medical Claims
Claim adjudication under most health schemes remains largely manual, leading to
High administrative load on health systems
Errors or inconsistencies in adjudication
Slow claim approvals
Manual, repetitive data entry
Medical data must be extracted from diverse, unstructured documents, lab reports, discharge summaries, blood test results submitted by healthcare providers. This complexity slows down the claim process.
Why Solving This Matters
Automating claim adjudication offers transformative benefits
Faster reimbursements for hospitals
Admins can focus on complex, high-impact cases
Claimants face fewer delays
Scalability and consistency as claim volumes grow
Our Solution
We’ve built an AI-powered system that automates the claims adjudication process. It uses document intelligence techniques . This enables faster, more consistent, and scalable decision-making in claim processing.
Cross-verify details across documents to ensure they match the requirements of the treatment package(s)
Extract key clinical and administrative parameters from submitted medical documents
Raise automated queries if information is missing or inconsistent
Auto-adjudicate claims by applying predefined rules on extracted information
This enables faster, more consistent, and scalable decision-making in claim processing.
Benefits
Streamlined Claims Adjudication
Reduces manual errors and brings consistency with standardized, digital-first workflows for faster, more reliable processing.
Automated Claim Processing
Uses AI tools to automate routine claim approvals, easing administrative load and improving speed and accuracy.
Faster Claim Turnaround Time
Benefits for Everyone

Who can use it ?
This solution is designed for public and private insurers involved in healthcare schemes, third-party administrators (TPAs) managing insurance claims, GovTech partners aiming to integrate AI into healthcare workflows, and researchers or developers exploring the application of document AI in real-world public health scenarios.
Government
Better oversight, cost savings, and scalable operations
Tech Ecosystem
Faster processing means quicker access to care and fewer claim rejections
Bigger Picture
Our larger mission is to modernize and simplify public healthcare delivery through AI. By open-sourcing the system, we aim to foster adoption across healthcare ecosystems in India and beyond, encourage collaborative improvements from developers and researchers, and support governments in building resilient, digital-first health infrastructures.
Patients
Faster responses, better services, and greater clarity on issue status
Hospitals
More visibility into system gaps and better insights for decision-making
Performance Indicators
Manual Review Time
Monitors how much time is saved by reducing manual claim checks
Daily Claim Volume
Measures number of claims processed daily vs. historical trends
Claim Turnaround Time
Captures total time taken from claim submission to resolution
Adjudication Consistency
Evaluates uniformity in decisions for similar claim types
Peak Load Handling
Assesses system performance under high-volume claim spikes
Query Resolution Efficiency
Tracks the rate of system-suggested clarifications or queries
User Feedback (NPS)
Measures satisfaction of claim processors and administrators
Data Integrity Compliance
Monitors % of claims that meet complete adjudication standards
Claims Auto-Adjudicated
Proportion of claims processed fully without manual intervention
False Approvals / Rejections
Checks for incorrect decisions—either overly strict or lenient
Reimbursement Time
Measures time taken to reimburse hospitals post-adjudication
System Availability
Uptime and responsiveness across regions
Product Demo & Visuals
Technical Architecture
How it works
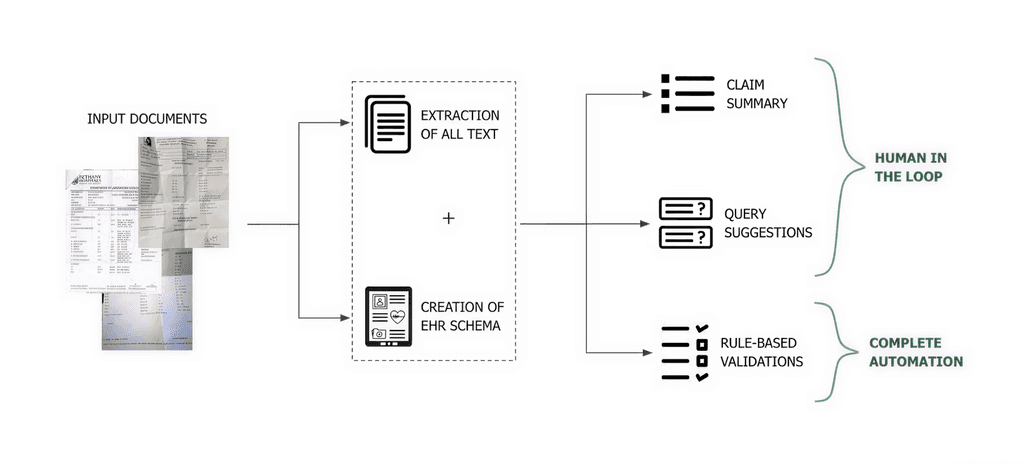
Potential Methods for Claim Auto-Adjudication Automating Document Processing
Document Ingestion
All submitted medical documents are scanned into the system
Information Extraction
Uses NLP & vision-based models to pull details -patient condition, procedures done, discharge notes, etc
Package Matching
Extracted data is cross-checked against the claim’s proposed treatment package(s)
Summary Generation
A structured, human-readable summary is created for each claim
Automated Decisions
Claims are either approved, rejected, or flagged for further review based on eligibility criteria
How to Use
Pre-requisties
(Languages, libraries, system requirements)
Python
Version 3.8+
Storage
10 GB+
Usage Guide
Follow these steps to use the system
Configure input source in
config.yamlRun the service using
python serve.pyAccess the web interface at
http://localhost:8000Upload documents or connect to API endpoints
Usage Guide
Follow these steps to use the system
Clone the repository:
Follow the instructions within each tool's directory to install necessary dependencies and configure the tool.
conda create -n doc_env python=3.8
conda activate doc_env
Install all the dependencies
cd doc_intelligence
pip install -r requirements.txt
Opportunities for colloboration
We encourage contributions to
Developers to improve form parsing accuracy and model performance
Domain experts to validate outputs in real-world healthcare settings
Health programs to pilot tool with varied public health forms
Contributors to test and refine deployment workflows
Inner-Source Info
Coming Soon…
Contributors
Team or Contributors
Nevil Vekariya
Associate ML Scientist - II
Sudharshan Sekhar
Machine Learning Scientist
Contact Persons
Nevil Vekariya
Associate ML Scientist - II






